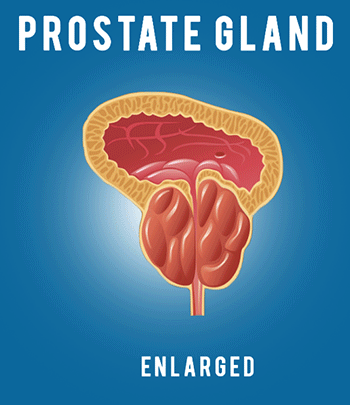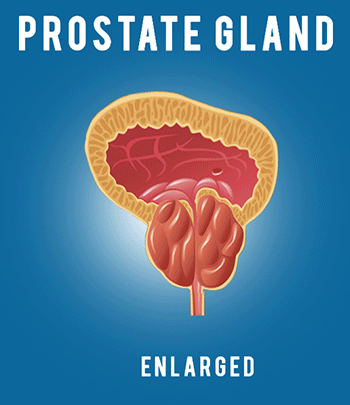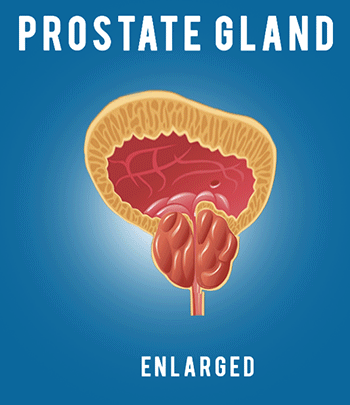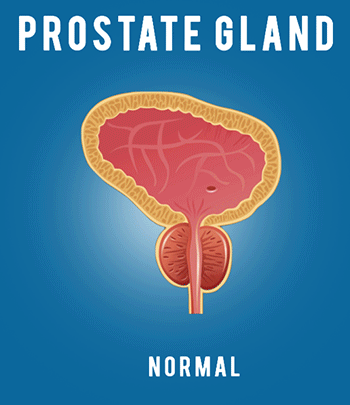
Viewing prostate cancer aggressiveness in a unique way
So magnetic resonance imaging is a technique that’s used very commonly in a clinical setting in order to be able to diagnose disease, as well as evaluate response to therapy. In the conventional sense, one usually looks at just the anatomy, but in the methodologies that we’re working on, we’re trying to look at tissue metabolism function in order to be able to understand what happens in a cancer when a cancer progresses, and also when a cancer responds to therapy. The first application of this technique is to patients with prostate cancer. It’s very difficult right now because it’s easy to find out that somebody may have a tumor, but it’s not very easy to know whether it’s going to be an aggressive tumor. So we’re using this new technology to be able to evaluate the aggressiveness of the tumor in order to be able to decide whether we get to treat now or treat later, or even when we’re giving a particular therapy, whether that therapy’s working, or whether it’s changing the way that the tumor is progressing and is actually having a good effect or not. It’s the first time that we’ve actually applied it to humans. This particular technology is novel in the sense that we’re taking a metabolite that is specifically labeled, and we’re essentially exciting it in a special way, and delivering it directly to the patient. And as that molecule goes back to its original state, it releases energy, and that energy can be picked up by the MRMI scanner, and then get translated into imaging and particular metabolic data that we can further analyze in terms of tumor aggressiveness. We actually place this compound into a very strong magnetic field at a very, very low temperature for a given period of time, and then after that material is polarized we’re able to dissolve it into a solution so that it can be injected into the patient. And the expiration date, so to speak, of this particular substance is very short, on the order of seconds, so all of this takes place pretty rapidly. From the patient’s perspective, they don’t really notice anything different from any other sorts of traditional MRI scans. They’ll move into the MRI scanner room with an IV in place, with some IV fluid, they’ll actually get placed into the MRI scanner where initial imagines will be taking place while we are finalizing and preparing the compound, and then when it’s ready for administration the patient’s already in the MRI scanner, it gets administered from the outside by the nurse. This happens over a period of minutes, and then after we’re done acquiring the imaging the patient gets pulled out of the MRI scanner, and then we just monitor some vital signs afterwards. I think that there are really four big parts of this technology which require that a lot of different people come together. There’s the first part which is what is the disease, and what is the biological process that is of interest; therefore, what is the compound that you want to design, and how would you design the experiment? And that requires chemists, clinicians, people that are developing new drugs. Then there’s the next part which is the physics and the polarizer; the design of the instrumentation, which has really required the industrial collaboration, as well as the expertise of the engineers here. The third part is the MR scanner itself, and actually making the scanner obtain the signals that you want in order to be able to get the appropriate images. The fourth part of this is really working with the clinician in order to decide how to use the technology in the best possible way that will benefit patients. The expertise that I’m bringing to the project are my mathematical skills. My background is in mathematics, but I am trained as a bioengineer as well, so I can work on applying technology to medical problems or biological problems. I’m specifically bringing my software skills to understand how to acquire and analyze the data that’s being obtained. My particular contribution to this clinical trial has to do with the formulation and design in terms of this investigational medicine. Any time you have a clinical trial, pharmacy needs to be involved, not only for the traditional standpoint of dispensing the correct medicine to the patient, but also from a regulatory standpoint and a quality control standpoint, to make sure that what we’re actually administering to the patient is acceptable for humans. Here at UCSF is really a place where we can collaborate, and where we understand how to collaborate well across different disciplines. We’ve taken really two independent fields and brought them together – the imaging and bioengineering side, in addition to the sort of pharmacy and formulation side – and brought them together to streamline this clinical trial. So we’re really excited. I think there are many years worth of work for us to continue.