Pharmacology – ACNE TREATMENTS (MADE EASY)
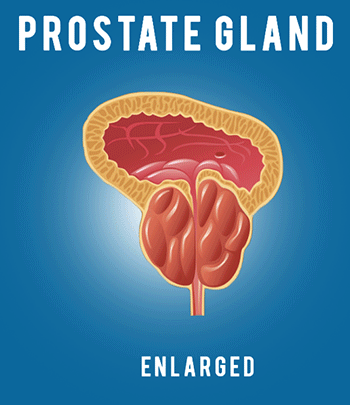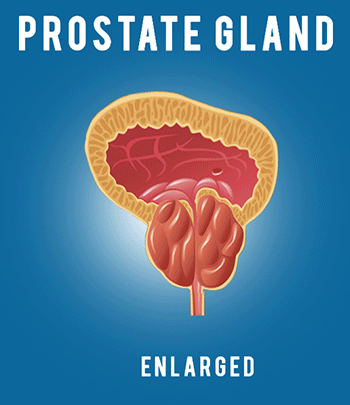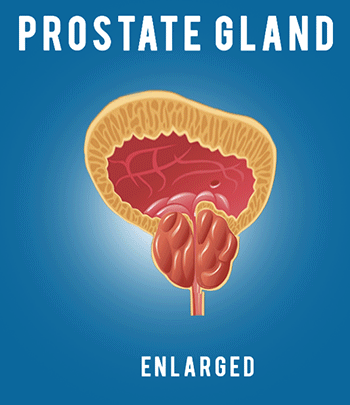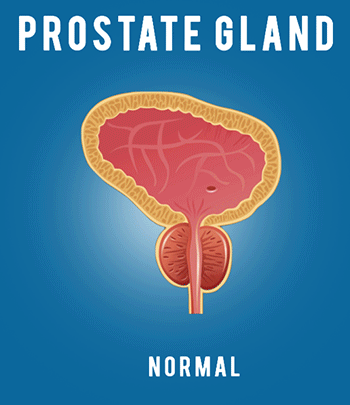
In this lecture we’re gonna cover the pharmacology of drugs used for acne treatment. So let’s get right into it by first discussing the pathophysiology of acne. Acne is a multifactorial inflammatory disease that affects the skin’s oil glands and hair follicles. The oil-producing glands present in our skin, known as sebaceous glands, are usually attached to hair follicles and release a fatty substance called sebum that helps protect and lubricate the skin and hair. Acne occurs when sebum and dead skin cells become trapped in a hair follicle, thus forming a small plug known as microcomedo. Overtime as sebum and dead skin cells accumulate in the blocked pore, microcomedo may enlarge to form an open comedo knows as blackhead or closed comedo knows as whitehead. Now, there are three major factors thought to be important in the pathogenesis of acne. The first one is overproduction of sebum. The second one is follicular hyperkeratinization. And the third one is presence of acne-causing bacteria that includes various strains of Propionibacterium acnes, abbreviated as P. acnes. Now let’s discuss these a bit more… So, overproduction of sebum is generally the result of excessive growth and activity of the sebaceous glands, which leads to clogged pores that trigger spots of inflammation. The most common causes affecting activity of sebaceous glands include (1) Genetics. Our genes influence the size and activity of the sebaceous glands. So the larger and more active the glands are, the greater the chance of developing acne. (2) Hormonal changes: for example, at puberty, the body begins producing more androgen-type hormones, which cause the sebaceous glands to enlarge and produce more sebum. Now, let’s move onto to the second major cause of acne that is follicular hyperkeratinization. So hyperkeratinization occurs when the cells of the follicle become cohesive and do not shed normally onto the skin’s surface. As a result dead cells tend to clump together, blocking pores and causing a backup of sebum in the follicle. Moving on to our third major cause of acne that is prevalence of acne-causing bacteria, specifically P. acnes that thrives in the oily depths of our pores. The airless environment that results from the formation of plug in the hair follicle causes the bacterium to proliferate and turn sebum into fatty acids that in turn activate inflammation in nearby skin cells. Now, let’s move on to discussing the mechanism of action of drugs used in treatment of acne. The available pharmacotherapeutic options can be divided into three main groups; (1) Retinoids, (2) Antimicrobials, and (3) Hormonal Therapy. So let’s discuss these one by one starting with Retinoids. Retinoids are a class of compounds derived from vitamin A or having structural or functional similarities with vitamin A. Their main targets are epidermal cells known as suprabasal keratinocytes. Upon entry into cells, if needed, retinoid first gets converted into its biologically active form that is retinoic acid. Retinoic acid is then shuttled by cellular retinoic acid binding protein (CRABP) into the nucleus where it binds to either the retinoic acid receptors (RARs) or the retinoid X receptors (RXRs). These retinoic acid bound receptors then bind to, so called, retinoic acid response elements on target genes causing activation of transcription factors. These, in turn, activate the synthesis of heparin-binding epidermal growth factor (HB-EGF) and amphiregulin (AR), which through the interaction with epidermal growth factor-receptor (EGF-R), cause proliferation of basal keratinocytes, thereby inducing thickened epidermis. Through this action, retinoids promote shedding of keratinized mature and dead skin cells at the surface, which leads to expulsion of mature comedones and suppression of microcomedo formation. The examples of topical retinoids are Tretinoin, Adapalene, and Tazarotene. Now, in general all retinoids share the same mechanism of action, however, unlike the topical agents, oral retinoid called Isotretinoin has additional unique inhibitory activity on the sebaceous glands. That is, it inhibits the proliferation and differentiation of sebum-producing cells, thereby shrinking the sebaceous glands and decreasing sebum production. In addition to that, oral Isotretinoin also reduces colonization with P. acnes and the number of leukocytes that aggregate at the inflamed site thereby reducing the number of infected and inflamed comedones. Now, when it comes to side effects topical agents are known to cause skin dryness, irritation, redness, swelling, blistering, and sensitivity to sunlight. Oral Isotretinoin, on the other hand, is much more potent medication than topical retinoids and thus is associated with more severe side effects that include mood changes, muscle or bone pain, and gastrointestinal disorders among many others. Furthermore, isotretinoin is known to cause birth defects and thus should be absolutely avoided in pregnancy. Now let’s move on to our second group of drugs used in treatment of acne that is antimicrobials. So drugs that belong to this group target P. acnes, a gram-positive bacterium that is involved in the pathogenesis of acne. As you may already know the drugs of choice for this, are antibiotics. The most commonly used antibiotics for acne include Sulfamethoxazole and Trimethoprim, which block two consecutive steps in the biosynthesis of tetrahydrofolate that is needed by bacterial cells for eventual production of DNA, RNA, and amino acids. Other antibiotics include Clindamycin, Doxycycline, Minocycline, Erythromycin and Azithromycin, which disrupt bacterial ribosome to inhibit protein synthesis. Ultimately all of these antibiotics inhibit the growth of susceptible P. acnes as well as reduce inflammation, which helps to clear acne. For more detailed explanation of these and many other antibiotics check out my video dedicated to pharmacology of antibiotics. Now, when it comes to side effects, if antibiotic is taken orally, most common complaints include nausea, vomiting and diarrhea. On the other hand if antibiotic is applied externally to skin, the common adverse reactions may include dryness, redness, and itching. Now, unfortunately overuse of antibiotics can promote the growth of resistant bacteria, which can make treating acne more challenging. To limit the resistance, topical agent called Benzoyl Peroxide is often prescribed either alone or in addition to antibiotics. So Benzoyl Peroxide reduces the likelihood of developing antibiotic resistance due to its unique mechanism of action, which involves release of free oxygen radicals into the pores. Since P. acnes bacteria cannot survive in an oxygen-rich environment, it gets killed by direct toxicity. In addition to its antimicrobial properties, Benzoyl Peroxide appears to have an anti-inflammatory action, as well the ability to speed up the turnover rate of epithelial cells, thereby promoting resolution of comedones. When it comes to side effects, because Benzoyl Peroxide is applied directly to skin, common complaints are similar to other topical acne treatments and include dryness, redness, itching, and burning. Now let’s move on to our last group of drugs used in treatment of acne that is hormonal therapy. As we have learned so far, sebaceous glands and sebum production play a central role in acne formation. They also happen to be regulated by androgen hormones. Majority of the circulating androgens are produced by gonads and the adrenal gland, however they are also produced locally by sebocytes, which are the major cell type in sebaceous glands that secrete sebum. Now, sebum production is mainly regulated by dehydroepiandrosterone-sulfate abbreviated DHEA-S. Although DHEA-S is considered a weak androgen, the sebocytes have required enzymes to convert it into stronger androgens, starting with androstenedione, then testosterone, and finally the strongest one, dihydrotestosterone. Despite their formation within the sebocytes, these androgens can also be absorbed from the outside. Once inside the cell, testosterone and dihydrotestosterone bind to the cytoplasmic receptor to form complex which then enters the nucleus and binds to specific gene, thus initiating cellular responses that lead to sebocyte proliferation and enhanced sebum excretion. Now the problem arises when the level of androgen hormones, such as testosterone, increases, for example during the puberty period. This can lead to overstimulation of androgen receptors, which in turn can result in excessive sebum production, subsequent clogging of the pores and formation of favorable environment for the growth of P. acnes bacteria. Now, to mitigate this problem, agent called Spironolactone is used due to its ability to block the androgen receptors within sebocytes and thus inhibit androgen-induced sebocyte proliferation. Now, just like increase in hormones during puberty can trigger acne, hormonal changes in females, such as those relating to menstrual cycle, can also affect breakouts. The main culprit in this case appears to be the low or changing levels of estrogen, which leads to increased testosterone to estrogen ratios during specific segments of the menstrual cycle. Estrogen is thought to suppress sebum production by directly opposing the effect of testosterone as well as inhibiting testosterone secretion. In addition to that, estrogen increases production of sex hormone-binding globulin, abbreviated SHBG which is a protein that regulates certain hormones including testosterone and dihydrotestosterone, by binding them and making them unavailable for cells to use. So another option for treating hormonal acne is to alter the natural female reproductive cycle with the use of oral contraceptives that work by few different mechanisms. Firstly, the estrogen component of hormonal contraceptives works to boosts levels of sex hormone-binding globulin thereby decreasing levels of free testosterone. Secondly, oral contraceptives suppress luteinizing hormone production by the pituitary gland, which in turn decreases androgen synthesis by the ovaries. And lastly, oral contraceptives inhibit 5α-reductase, which is the enzyme responsible for the conversion of testosterone to the most potent and active androgen, dihydrotestosterone. Now the most commonly used oral contraceptives have low doses of synthetic estrogen, Ethinyl Estradiol, combined with differing progestin components. Because synthetic progestins have androgenic activity that may exacerbate or trigger acne, it’s prudent to select oral contraceptive that contains a progestin with low androgenic properties such as Norgestimate or Desogestrel. Now, when it comes to side effects, Spironolactone can cause increased urination, irregular periods, and breast tenderness. On the other hand, side effects of oral contraceptives can include nausea, headache, breast tenderness, breakthrough bleeding, weight gain and increased risk of blood clots. And with that I wanted to thank you for watching I hope you enjoyed this video, and as always, stay tuned for more.