Prostatic artery embolization: A non-surgical treatment for enlarged prostate | UCLAMDChat
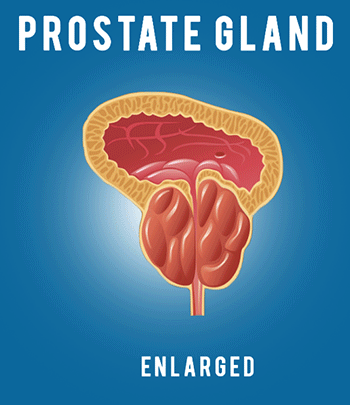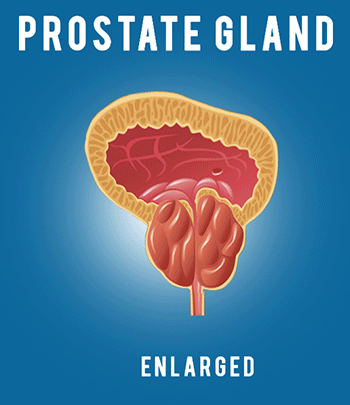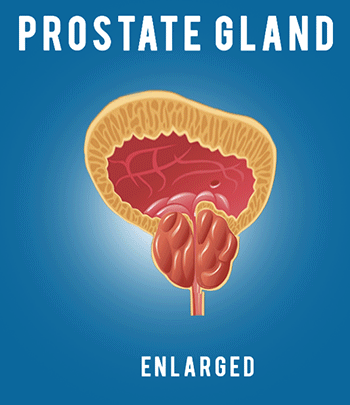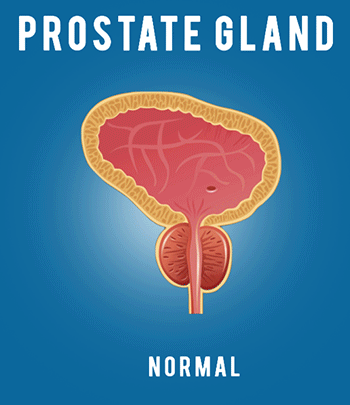
Hello, my name is Justin McWilliams, and I’m an interventional radiologist here at UCLA. Today, I’m going to be discussing a minimally invasive treatment option for BPH called prostatic artery embolization, or PAE. If you have any questions about any of the content of this video, or if you’d like to learn more, please call this number on the screen, or you can email me directly at the email below. Before we talk about the PAE procedure itself, it’s helpful to have a little background information about the prostate. The prostate is a walnut-sized gland which is situated beneath the bladder. The prostate surrounds the urethra, which is the tube that carries urine out of the bladder during urination. As men age, the prostate enlarges. This process is referred to as benign prostatic hyperplasia, or BPH. This refers to the growth of glandular tissue in the prostate, which can compress the urethra and restrict the flow of urine. It’s an extremely common condition in older men, affecting about 50% of men over the age of 50 and about 70% of men over the age of 70. Symptoms of BPH are multiple and can include weak stream, frequent urination, straining, inability to completely empty the bladder, and waking up at night to urinate. Traditional treatments for BPH include lifestyle modification, such as urinating immediately when you feel the urge to urinate, reducing fluid intake before bedtime, and reducing the intake of alcohol and caffeine. As symptoms progress, medical management may be considered. This includes the use of alpha blockers, such as flomax, and 5-alpha reductase inhibitors, such as finasteride. These are effective, but the degree of symptom improvement that they produce is relatively modest. For more severe urinary obstruction, urologists may recommend transurethral resection of the prostate, or TURP. During this procedure, a scope is passed through the penis and into the prostate to core out some of the prostatic tissue to increase the size of the channel through which urine can flow. This is the gold standard surgical treatment for prostates measuring up to 80 to 100 ccs, and it’s fairly effective. It’s been used for many years and is known to be very durable and good at reducing symptoms. However, there are possible side effects and complications which can occur with that treatment for patients who have a particularly large prostate. Sometimes, surgical prostatectomy is recommended. This refers to complete surgical removal of the prostate and is typically used for prostates that exceed 80 to 100 ccs in size. Again, it’s extremely effective and is well known to improve urinary function. However, certain side effects and complications can occur. In the end, millions of men continue to suffer from the symptoms of BPH, either because they’re fearful of the side-effects of surgery or because they may not qualify for surgery, either because they’re advanced in age or perhaps they have multiple coexisting medical conditions. Now, that brings us to our treatment that we’re going to discuss today, which is prostatic artery embolization. Now, embolization refers to the blockage of blood flow in an organ or a blood vessel, and embolization procedures have been performed by interventional radiologists for many years, either to block blood flow to tumors to shrink them, or to stop bleeding. In more recent years, this same technique has been applied to the prostate. The prostate is a rather vascular organ, and it receives its blood supply from a prostatic artery, usually one on each side of the pelvis. If we’re able to access into that prostatic artery and block it, we can reduce the blood flow into the prostate. As we stop the blood flow, we can shrink the prostate and relieve the compression on the urethra. So, how is this done? Well, the procedure is done in an angio suite, and it’s done under minimal sedation, which means you hardly need any sedation at all, just some local anesthesia. The entire procedure is done through a small sheath, which is placed into the artery we use for access, either a small artery in the wrist or the artery of the upper thigh. No incisions are needed, and the entire procedure is done under x-ray guidance. Once the sheath is placed, a small catheter is passed through the arteries of the pelvis and used to navigate into the pelvic artery. An angiogram is performed, and an angiogram refers to the injection of contrast dye through that catheter, which makes a picture of all of the blood vessels of the pelvis. The interventional radiologist uses that picture to find and locate the prostate artery. In this case, the prostatic artery is identified by the white line. Once that prostate artery is localized, a tiny micro catheter measuring less than one millimeter is navigated into the prostatic artery. An additional angiogram is performed to confirm the correct position. You can see in this angiogram the passage of blood flow into the vascular prostate, which is causing it to light up with this blush. Once we’ve achieved proper position in the prostatic artery, small particles are injected through the micro catheter until we block the blood flow into the prostate. Once the blood flow is blocked, we confirm the complete occlusion of that vessel with an additional angiogram, and we then withdraw the catheter and then navigate into the pelvic artery on the opposite side. We then advance the micro catheter into the opposite prostatic artery, and we repeat the embolization process. Once the embolization process is completed, then the catheter and sheath are removed, and the pinhole access into the artery is closed. The entire procedure takes about 2-3 hours, and following about 2-3 hours in the recovery area, patients are discharged home the same day. Over the following weeks, the prostate, now deprived of its blood supply, begins to shrink, and as the prostate shrinks, the urination improves. There are several advantages of PAE and its use for BPH. It’s an outpatient procedure not requiring admission into the hospital, it’s almost completely painless, requiring only some conscious sedation and local anesthesia, no Foley catheter is required at any point during the procedure, the recovery from the procedure is rapid, and the safety profile is very good, including a lack of urinary incontinence, minimal blood loss, and a maintenance of sexual function. So, how are the results? Well, over a study of more than 2,000 patients that have had the PAE procedure, we’ve seen significant symptom improvement, and at least 80% of individuals, the degree of improvement is typically intermediate between that found with medication and that achieved with traditional surgery. There’s also a significant improvement in the patient’s quality of life related to urination. The side effects are mild, frequently, a week’s worth of bladder or urethral irritation can occur, but bleeding and infection are uncommon, and major complications are very rare, occurring in less than 1% of cases. PAE is unique because it is a minimally invasive procedure. Because of that, patients who may not be candidates for traditional surgery may be good candidates for PAE. This includes patients with advanced age, patients who have multiple medical problems, and patients who are on blood thinners and can’t come off of them. Also, it applies well to patients who wish to avoid surgery because they’re concerned about the possibility of complications or side effects. There are also some specific circumstances where PAE can be particularly useful. The first is the presence of an indwelling Foley catheter. Some patients have very severe urinary obstruction, so much so that they have to live with the Foley catheter indwelling in the bladder. These patients are often not surgical candidates, and in those cases, we’ve been able to achieve catheter independence and actually remove the Foley catheter with return of spontaneous urination in about 80% of cases after PAE. Secondly, patients who have bleeding from the prostate can definitely benefit from PAE because we block the blood flow into the prostate. During the procedure, we’re able to reliably reduce or eliminate bleeding. Finally, patients with very large prostates, over 80 to 100 ccs, often are limited in traditional surgical techniques that they can have, but PAE actually works better the larger the prostate is. Usually, the bigger the prostate, the larger the prostatic arteries, and therefore the greater our ability to navigate into the arteries and block them. Thus, there’s no upper limit to the prostate size which we can treat with PAE. There are a few limitations of PAE for BPH. Not every patient will improve after the PAE procedure. It does depend on the presence of intact bladder function for normal urination to occur. Also, the prostatic artery embolization procedure is rather technically challenging, and it does require us to navigate into the small prostatic arteries. In some cases, atherosclerosis may make those arteries very difficult or impossible to access. Secondly, PAE may not improve urinary obstruction as completely or as quickly as traditional surgery can. Finally, smaller prostates may be more difficult to treat with PAE and may be better treated by traditional techniques. Work up for prostatic artery embolization begins with the clinic visit and evaluation on the same day. We may do an imaging study, such as a CT angiogram of the pelvis. This is a specialized, non-invasive imaging study that can show us the size of the prostate as well as show us the size and course of the prostatic arteries. We work closely with urology for this procedure. Although we can perform a prostatic artery embolization, we’re by no means a replacement for a urologist. We rely on urology to evaluate for other causes of urinary symptoms other than BPH. Also, urology can offer traditional therapies, both medical and surgical, as well as a variety of minimally invasive surgical options. If you don’t have a urologist, we have a world-class urology department here at UCLA, and we’d be happy to refer you to one. In conclusion, prostatic artery embolization is both effective and safe in the treatment of benign prostatic hyperplasia. It offers a minimally invasive way of treating BPH without surgery, and it may be able to fill an important gap between medication and traditional surgical treatment. If you have any additional questions or would like further information, please call our UCLA interventional radiology clinic or feel free to email me directly at the email below. Thank you very much.