Best Outcomes in Surgery for Prostate Cancer – Christopher Saigal, MD | UCLAMDChat
Surgery for proste cancer
Surgery for prostate cancer – here are tips on how to get the best outcomes when having surgery for prostate cancer.
During this webinar, if you have questions, feel free to ask them on Twitter at the hashtag #UCLAMDChat or comment on YouTube. So if you’re watching, you may have decided or are considering about having surgery for prostate cancer, and this is a tough choice. You’ve probably had a lot of discussions with friends and family and certainly your doctors about this. It’s tough because there are competing goals and values you have to consider when deciding about surgery.
Some of the more important ones that many men consider are returning to their sexual health baseline after treatment. This is probably the most variable thing for some men. This is very important for some men, not as important, and men’s sexual health baseline in their 50s and 60s vary quite a bit. Most all men find retaining control of their urinary function to be very important. As a side note, prostate cancer surgery can also help men who have blockage or straining to urinate by removing that tissue. A key goal for almost all guys is being cancer-free. Of course, you’re having treatment to get rid of this cancer, and you don’t want it to come back.
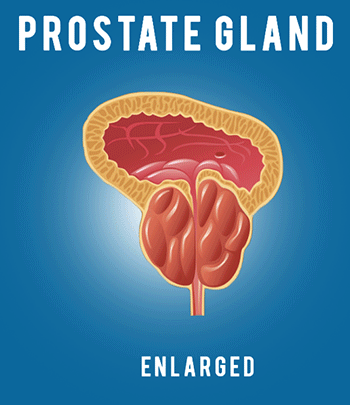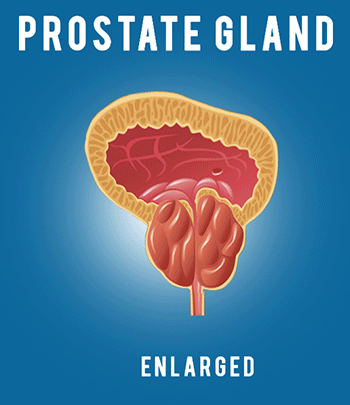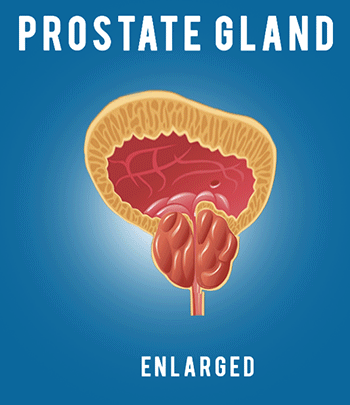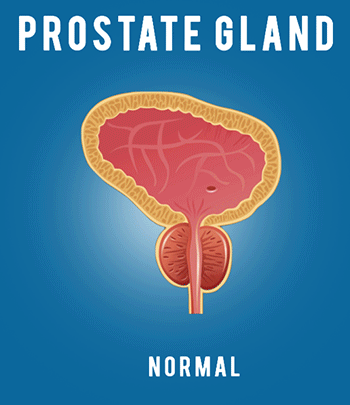
And finally, men want to get back to their normal life as soon as possible, work, recreation, family, and so forth. So your surgeon will certainly help you in maximizing these outcomes, but there are some things that you can do in terms of engaging, asking questions, and doing your homework, in terms of getting the best outcomes. But first, why is this so complicated? Why are these things so interrelated? As a brief review, it’s because of the anatomy. So this is the prostate gland right here. It’s part of the male reproductive system, and its job is basically produce the fluid in the ejaculate that helps the sperm to live and initiate a pregnancy.
More prostae information is here.
__________________________________________________________________________________________________________________________________________________________
So, for many men, when they’ve been diagnosed with prostate cancer in their 50s or 60s or 70s, that function is not so important anymore, so it isn’t doing a whole lot for you. However, removing it does risk important things that you do care about, so, for example, these yellow structures are the nerves that come down from the brain and end up innervating the penis, so they don’t cause the sensation of the penis, but they trigger the arteries in the penis to open up and possibly fill with blood during sex, giving you an erection. So you can see here, these nerves live right on the surface of the prostate gland, and when you take that gland out, you’ve got to sweep those nerves off very carefully– that’s called nerve sparing–in order to preserve normal sexual function.
Sometimes the cancer is right at the surface there, and the nerve can be involved, and if you save that nerve, you could leave cancer behind. The second issue is that this thin tube here going through the penis, called the urethra, allows the urine from the bladder to come out the prostate, sits right in the middle there, and the urethra goes through it like a hole in the doughnut. So when you remove the prostate, you’ve gotta sew the bladder to the remainder of the urethra,
It comes down just fine but take some time for things to heal up down there, and you can leak urine for awhile after surgery as a result. So, how about sexual health? How can you maximize your outcomes? There are some things you can’t control, like your baseline sexual health function–some men are using Viagra or having weak erections on Viagra–and that predicts how well you’ll do after surgery. The best outcomes are for men who have excellent sexual health, good erections off of Viagra, other medical conditions can affect things, diabetes, high blood pressure can affect the health of the penile arteries.
You can, of course, optimize your diabetes control, optimize your blood pressure control before surgery to try to improve things that’s very important, and your age also predicts how well you’ll do in terms of sexual health after surgery, so older men tend to have a lower chance of getting back to their baseline than younger men, say, men under 65. But there are some things that you can take action on, perhaps help. One of these is learning whether nerve sparing is possible, and the other is the post treatment rehabilitation approach to sexual health. The final thing is surgeon experience. So, is nerve sparing possible? So, there are many surgeons. They determine this based on the physical exam of the prostate gland–that is, looking for nodularity there that implies that the cancer is involving the nerves.
They will use calculators that say what’s a chance, based on the person’s PSA and aggressiveness score, that the tumor is at the lining of the prostate or not. And also, during surgery, see if the nerves can peel back easily or if there’s evidence that it’s kind of sticky, as a way to judge whether the cancer is involved. A newer way to assess the risk of, you know, whether nerve sparing can be done is using preoperative MRI of the prostate gland. There’s been several studies on this, and one study looking at all the existing studies, called a meta-analysis, concluded that preoperative MRI changed the plan, in terms of nerve sparing, in about 1/3 of the men.
And in those cases, essentially perhaps half of them, the nerve was spared when it was going to be taken, according to initial surgeon experience–that’s given men a better chance to get sexual health back, and in half the cases, the nerve was taken because the MRI indicated the cancer had extended into the nerve where the surgeon was not thinking it had, which results in better cancer control. So, some caveats with that. MRIs are not uniform, so the quality of MRI does vary by where you get it and by the experience of the radiologist who reads the MRI for the surgeon.
So if you inquire about getting a preoperative MRI, you should make sure that the surgeon is sending it somewhere where they do a lot of them and the radiologists are familiar with them, because there’s about a 50/50 chance that radiologists would disagree about prostate MRI findings, so you want to go somewhere with a lot of experience. Regardless of that, ones that I did find that in one in four patients who had nerves taken, that they could have been spared, had the MRI been used to guide decision-making.
So, it can be helpful, and one other caveat is that if you’ve had a biopsy already, and it was not done with the help of MRI guidance–and you can get an MRI right after your biopsy–you have to wait for 2-4 weeks for the bruising in the prostate to go down so that there are better pictures obtained for the radiologist. Another way you can take action, perhaps, help yourself, is asking about penile rehabilitation, it’s called.
This is a formal program to try to maximize the chances that the nerves will function after surgery. Even if the nerves are spared, when they’re pushed off the prostate, they’re stretched and the word for that is neuropraxia, and it takes a while for the nerves to recover from that stretching injury. They heal at a micron per day rate, so you have up to 12 months to really get your full sexual health back, and during that time, you can do things to improve your chances of getting sexual activity back in your life.
There are many protocols in this regard. Most of them start with a low dose of what’s called a phosphodiesterase-5 inhibitor, which is like a Viagra or Cialis, it doesn’t really matter which one–it isn’t the dosage that we would use to have you get an erection. It’s really a low dose to try to allow for better recovery of the nerve and also for better penile health, in terms of reducing scarring in the penis.
You might know that when a nerve is damaged at the muscle, that its supplies can become withered away, and similarly, if a nerve is stretched, the penis can have changes in its architecture and make the ability get erection worse, even if the nerve heals back completely, so we think these drugs help the penis stay healthy and avoid scarring inside the penis. They also will use vacuum devices, basically pump devices that mechanically let you have an erection to prevent the scarring process, and some men have to use injections of the small diabetic-size needle of a basically liquid type Viagra that gives you a really good erection.
One meta-analysis we’re looking at, all the studies in this area found that these types of protocols did improve the proportion of men who improved, in terms of sexual health, after surgery by a factor of two, but what’s less clear is whether those men have a better spontaneous erection rate when they stop these interventions–so the protocols do improve sexual health, it’s important to discuss with your surgeon what their protocol might be, or if they don’t know, to read about that and go on one, but yeah, we’re not clear about whether these things are going to give men the ability to be better active off of Viagra or Cialis.
What’s more late-breaking is that we have found that there’s evidence that prehabilitation before surgery can be helpful in this situation. So here at UCLA, Dr. Jesse Mills, our Men’s Health doctor, did a study where he enrolled about 100 men before surgery and began this protocol ahead of time with a low dose of Cialis and a low dose of an amino acid called l-citrulline, and they started this protocol, and he compared how these guys did with guys that started the protocol after surgery only, and they did better if he started ahead of time by a significant amount, so we’re now referring–almost all of our patients are interested for penile prehabilitation before surgery, and it’s something to consider if you are considering surgery. Another topic in sexual health is surgeon volume. So, it makes sense that the more of something that you do, the better you are at it, and nerve sparing is a delicate procedure that tends to improve, in terms of success, with volume.
That is not a hard and fast rule–there are studies that show that, you know, one study showed that in the top high-volume surgeons, about 8% of them were responsible in the top 1% of the complication rate, so surgeon volume is, directionally, the thing to look for–it isn’t a perfect guide to finding a good surgeon, but it’s certainly a good bit of information to have. It’s hard to pin down the exact relationship between surgeon volume and sexual health outcomes because most these days are done on using your insurance claim to say who was on pills or who was having surgery for problems after prostate cancer surgery, but a lot of guys don’t take pills and don’t have surgeries after this for these purposes, so you miss their experience.
One major medical center did a careful study where they asked men after surgery every 3 months how they were doing in terms of sexual health, and they did find that volume–okay, so I’m greater than a hundred cases–was associated with better sexual health outcomes, and their patients had also better urine health outcomes, less incontinence, and that both those outcomes tended to vary together without a sacrifice of cancer control, which is pretty convincing, but just to emphasize the topic here, this is that data from that study, and you can see here the average was 30% of probability of sexual health recovery at 12 months.
This is all comers, so basically, guys that started out with bad disease, that had their nerves taken, that are older, and guys that are younger, that had the nerve spared, so it’s kind of an average of everybody. Anyways, here is an individual surgeon. There’s a lot of variation in terms of how they did, but what they found was that when they did a subset analysis of just the surgeons who had over 500 lifetime cases, there was still this kind of variability, so it’s not a perfect guide, volume, but it’s something to ask about and think about in terms of urinary control. Surgery takes, as I mentioned, the prostate out, and the urinary sphincter muscle, which helps you control your urine when you cough or sneeze and have you not have an accident, needs to be sewn back to the bladder, and that muscle also takes time to heal and get strong again, and the typical way that we ask patients to take some action and improve their own health is by doing Kegel exercises after surgery.
Kegel exercises are exercises where you contract the muscles that you would use to hold your urine. So, if you could imagine you’re standing at a urinal and you’ve got to stop urinating, suddenly a fire alarm goes off or whatever, you would contract muscles deep in your pelvis, kind of near the rectal muscles, leave your abdominal muscles soft, and you hold that contraction for 10 seconds and let it go. There are a lot of different protocols on how often you have to do this after surgery, to contract these muscles. They vary mainly on the fact that it’s hard to remember to do this, and what’s the easiest way to get a guy to remember to do this? During the day, I tell patients hold it for 10 seconds and do it 10 times an hour while you’re awake.
The more you do, the better, basically. You should also do a Kegel after surgery when you stand up quickly, sneeze, or gonna laugh, that helps keep you dry, and definitely our data do suggest that people that follow-up protocol of pelvic rehabilitation in this area are more likely to recover urinary control. There is weaker evidence–and say that you can, if you do this before surgery, some patients are encouraged to start doing Kegels ahead of time–it’s not clear that actually helps, and for some patients, they’re referred to what’s called biofeedback after surgery, where electrodes are placed on the muscles, and they can see the contractions when they contract–it’s not clear that is always effective, but if patients have a hard time localizing the muscles or doing the exercises, we will often send to a physical therapist for further trainings. They specifically understand what to do, and physical therapists are often very good at teaching this, so depends on the person and motivation, but this is a great way to help you get back your urinary control. And again, this does vary by surgeon volume. This is data from that study. Y
ou can see that of the surgeons, there’s a wide variety in terms of how many men are controlling their urine at 12 months. Cancer control is a key outcome after surgery, and surgery experience does matter here. One of the best studies is about 8,000 patients and 72 surgeons, and that’s how they found that results plateaued after a surgeon’s done about 250 cases. So the patients that had the the lowest volume had about an 18% cancer recurrence rate–that means that their PSA became measurable again after surgery–versus 11% where the guys that had the most experience, or the surgeons have the most experience, after about 250 cases, and this is confirmed in several meta analyses, and this really brings us to the question of, how do you pick a surgeon?
This is a thing that you can do to maximize your chances, and, you know, there’s a few different domains to consider. First, of course, is the connection you have with the surgeon. Are you on the same page in terms of your goals? Is he or she listening to you? Critical, just gotta check. I think also volume is important, but with a caveat that volume isn’t everything. I think you can also look at whether your surgeon offers different programs for rehabilitation, considers that important, and makes it part of their practice, as an indicator of how important they see these things, and finally, the support services around the surgeon. Do they have a physical therapist at work?
Do they have a good radiologist to work with? Is there maybe clinical trials or a program for patients that are more complicated? Those are things to consider. Another thing that’s interesting to note is that we are in an age now where virtual reality is helping us operate better. This is an example of how we may be able to improve our outcomes. Here at UCLA, we have a new study where we’re using the patient’s preoperative MRI and plugging that data into our virtual reality model that we see during surgery.
So on this slide, it’s an example of what we would see when we’re using the surgical robot alongside the live version of the prostate, and the yellow, you see the nerves that are specific for this actual patient, and the red is where his tumors are, so with this, we can really get a sense of what are we looking at, and how does it relate to the patient’s MRI, and hopefully do a better job of sparing the nerves and also controlling the cancer. In a prior study, we did this in patients who had kidney cancers, and we noticed that there was reduced operative time, reduced blood loss, fewer complications, and better cancer control, as well as shorter length of stay. We’re hoping to find similar outcomes and make sense with our study here at UCLA on this topic. Finally, I want to talk about getting home and getting back to normal. So, a key parameter here is intraoperative blood loss.
Some surgeons offer this surgery as an open surgery, and some as a robotic surgery. I’d say robotic surgery is becoming quite dominant now, and with robotic surgery, one of the biggest differences is there is less blood loss, mainly because there is CO2 gas that’s put into the abdomen during surgery to sort of blow it up, we can see–and that puts pressure on all the veins that ooze from the prostate when we’re removing it, and that controls blood loss a lot better. When you have less blood loss, you have a faster recovery, you feel better after surgery and go home quicker. And finally, a really important point is the use of opioids after surgery.
You may have heard about the opioid epidemic in this country, and it caused many surgeons to look at their prescribing practices and see what’s really needed. Of course, our primary goal is to keep people comfortable, but we don’t want to have any side effects, so one study done recently found that 3/4 of the patients who had a robotic prostatectomy, the pain meds were never used, and so what that results is in a bottle sitting in your medicine cabinet.
That’s a key reason that other people can find it, take it, and it can be a problem. Another study found that in 84% of patients after the surgery, fewer than 15 oxycodone, say, are required. That’s about less than four days of pain medication. Opioids can be constipating, they can be addicting, and they can cause lethargy, and constipation can be a big problem after this kind of surgery, so we often will suggest, if your pain isn’t horrible, that you try a narcotic pain medication, and then 6 hours later try a Tylenol or Motrin, then go back to the narcotic and see if you can wean yourself off of it as soon as possible. And we try to prescribe fewer pills, that are in line with what people really use, to prevent the risk of someone else getting a hold of unused tablets. Well, thanks for watching, and I think we have some questions now that we can address.
All right, so one question is, “To find a surgeon with caseloads for 250+, is this data that doctors must share if I ask?” The answer is no, but I think that if a doctor doesn’t want to discuss it, that is a red flag. Most surgeons are aware of how many of these cases they’ve done, and these days I’d say that after the advent of robotic surgery, the proportion of urological surgeons doing the surgery is to drop, so the cases are happening in a smaller number of people’s hands, and those people tend to know how many cases they’ve done. “How long do you have to live with prostate cancer?” So that’s like a question about survival.
So, the good news is that prostate cancer is very slow-growing, and one large study from the UK found that in all comers, that 10-year death rate was around 1%, and this was even true in patients who had what’s called active surveillance. Of course, many of those people ended up on hormone therapy, but the chances of dying anytime soon are very low. The long-term horizon, though, of course, 15 or 20 years. This can be a cause of mortality, and so for men who have a longer life expectancy, treatment is indicated. “How do you determine using a surgical approach versus chemo?”
Well, chemotherapy is used for men who have a spread of cancer outside of the prostate gland. It goes all over your body, so that’s called metastatic prostate cancer. Surgery is used in patients where the cancer is just in the prostate, so we feel we can cure you by removing it. If you’ve got cancer elsewhere in your body, typically, taking out the prostate gland will not affect your overall survival. There are some studies on this topic, but they are pretty early days. “What causes prostate cancer, and how can I prevent it?” So, prostate cancer probably is a lot of genetics behind it. Some of these factors are things you really can’t control.
Your body accumulates changes in the genes as you get older because of various exposures, and we really don’t know how to exactly prevent at that level. In terms of dietary changes, things that are heart healthy tend to be prostate cancer healthy, so keeping a good body weight, a Mediterranean diet, keeping yourself physically active, and, you know, in large, population-based studies, those things are associated with less prostate cancer and better outcomes. There was one study about the Japanese diet, which is heavy in vegetables, and they followed patients as their families emigrated from Japan to Hawaii to the US, and the adoption of a Western diet seemed to increase the risk of prostate cancer in patients who had very similar genetic makeups.
And “How is prostate cancer typically diagnosed? Should I contact a urologist or an oncologist?” Well, prostate cancer is diagnosed by a urologist using what’s called a prostate biopsy, so what happens is we’ve got a blood test first, usually you got a test for–it’s called a PSA, or prostate specific antigen, if that’s abnormal or if your rectal exam result shows unnatural, your doctor will refer you to a urologist for a biopsy, and that’s done in clinic, and they will let you know what they find. Well, thanks for joining us today, and we look forward to you next time.
Google for more information on prostate health
or go to our home page