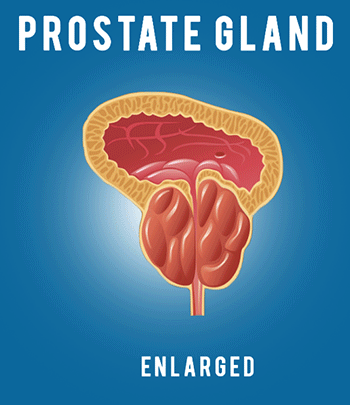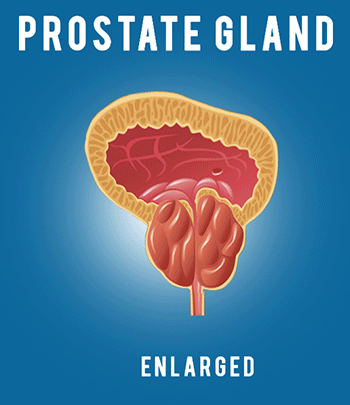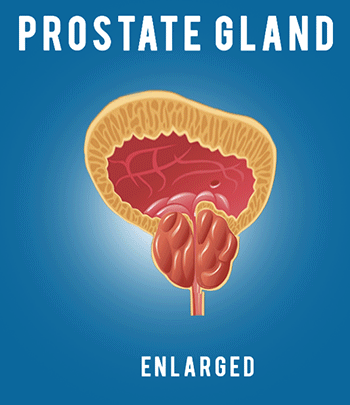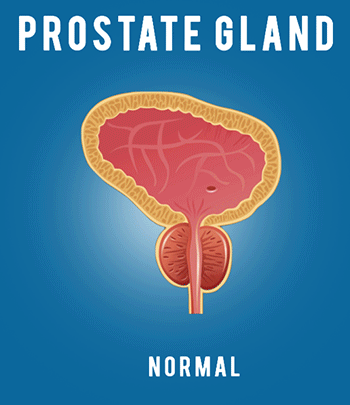
COVID-19: Infection Control Procedures and Protocols for Dentists
I think an important question we’ve allbeen asking ourselves in this last monthor two is as a dental professional is “whatcan we do?” I think it’s important foreverybody to be sure that they’reaccessing reliable information. we’re sofortunate that we have our professionalorganizations and our governmentagencies who are providing thatinformation and making sure that it’sthe most timely and the most accurate. Iwould suggest checking in with the ADAthe CDC, NIH, and OSAP websites on aregular basis and if you hear somethingthat you’re not sure is correct you cango and check those sources to confirm it. we really need to avoid panic and rumorsthere’s a lot of information beingcirculated that is inaccurate and in atime like this that can be dangerous. take the recommendations from your localstate and federal public healthofficials seriously and heed thenumerous calls to temporarily suspendall non-urgent dental appointments until this crisis is overand health officials indicate it’sappropriate to resume and they will giveus the types of recommendations thatwe’ll need to resume our operationssafely. so why do we need to stopelective procedures? we can’t reliablyidentify patients who are asymptomaticallyinfected, or who may be in thatincubation period. so we all need tolimit our contact with people outside ofour immediate circle for a while and ourimmediate circle is generally consideredto be our household contacts. many of ourdental procedures produce aerosols andaerosols are known to increase exposurepotential if patients are infected andthe virus is present in theirrespiratory fluids. we also know thatsupplies of PPE for treating sick peoplein hospitals is currently critically lowand if we use these fornon-urgent procedures we contribute tothe risk of our frontline healthcareworkers being left unprotected and theseshortages currently have no end date insight we’re not sure when that supplychain will be restored. the ADA came out with a great source andthat helps us identify which types ofprocedures we should continue to offerto our patients, the first are dentalemergencies. these dental emergencies arepotentially life-threatening and requireimmediate treatment to stop ongoingtissue bleeding alleviate severe pain orinfection, and they might include thingssuch as uncontrolled bleeding cellulitisor a diffuse soft tissue bacterialinfection with intraoral or extra oralswelling that potentially couldcompromise the patient’s airway. it alsoincludes trauma involving facial bonesthat potentially compromise thepatient’s airway. now urgent dental carewhich we also can provide focuses on themanagement of conditions that requireimmediate attention to relieve severepain or risk of infection and toalleviate the burden on hospitalemergency departments. these should betreated as minimally invasive aspossible so that means you’re avoidingmusic views of aerosol producinginstruments and devices and perhapsusing temporary materials to controlcaries that are causing pain to thepatient. urgent dental care includessevere dental pain from Popolinflammation pericarditis or third molarpain, surgical post-operative osteitis,and dry socket dressing changes. it alsoincludes includes abscesses or localizedbacterial infection resulting inlocalized pain and swelling. it could bea tooth fracture that causes pain orsoft tissue trauma, an avul or luxatedtooth from dental trauma andtreatment that was required prior tocritical medical procedures. also finalcrown of bridge cementations can be doneif the temporary restoration is lostbroken or causing gingival irritation. you can also provide care to patientswho have extensive dental caries ordefective restorations that are causingpain and you can manage these when theyhave to restoration techniques wheneverpossible such as solar diamine fluorideand glass ionomer. suture removals can continue to be doneas well as denture adjustments onradiation and oncology patients anddenture adjustments or repairs whenfunction is impeded and the patientcan’t eat. replacing temporary fillingson endodontic access openings andpatients experiencing pain and alsosnipping or adjustment of an orthodonticwire or appliance that’s piercing orulcerating the oral mucosa and biopsy ofabnormal tissues should continue. the CDCis providing constant guidance for usand how to safely treat patients andsafely be around other people when weabsolutely need to to provide thesevital services. these CDC guidelines arefound on their website and they shouldbe checked regularly because informationand needs are emerging and theseguidelines change as those evolve. rightnow the current CDC guidelines call thatdental providers should not provideelective procedures in concert with theADA recommendations. if you must treatemergencies ask screening questions forrespiratory infection, and if the patienthas a respiratory infection or is how tocontact with somebody who’s beendiagnosed with COVID-19 considerreferral to a medical center ifavailable and if that’s not possible andthe patient needs to be seen there’sstill some things that you can do andwe’re going to talk about those. andthere have also been some guidelinesthat have come out from the CDC foroptimization of PPE under the currentsituation where there is a shortage ofcertain things such as surgical masksthis is only to be used in thesecritical emergency situations and it isnot to be used for routine dental careor when PPE is available. these measuresinclude things like using a mask formore than one patient in some situationsand hospitals they are needing to dothis because there simply aren’t enoughmasks to treat all the patients. alsoduring this time any available in ninetyfive respirators should be prioritizedfor procedures that are likely togenerate respiratory aerosolswhich would pose the highest exposure ofrisk to health care professionals andthose are that is for patients who areconfirmed or suspected to have COVID-19,not for well patients. face mask protectthe wearer from splashes and sprays weshould continue to wear face masks andchange them between each patient or moreoften if they become wet. respiratorswhich filter inspired air offer agreater level of protection, they protectthe respiratory tract of the wearer. examples of procedures that producerespiratory aerosols are those likely toinduce coughing and the CDC identifiesthese as things such as sputum inductionand open suctioning of airways they donot address dental aerosols and thoseare not specifically mentioned inrespiratory aerosols. so this CDCguidance on optimization of PPE as Isaid things like reuse of a surgicalmask or a respirator is only after allother administrative and work practicecontrols have been exhausted. administrative controls do includethings such as providing only urgentcare, limiting people that are in thefacility, using telemedicine, and we’lltalk about that in a little, limiting the procedures in length and inthe spread of oral fluids and pleasevisit the CDC website where there is afull list of administrative and workpractice controls that can beimplemented to optimize the use of PPE.